Total Hip Replacements
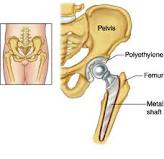
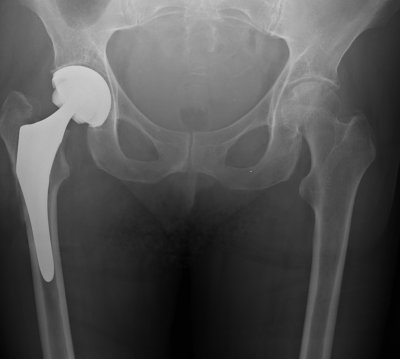
A Total Hip Replacement – or THR as we like to call it in this business – is a surgical procedure in which diseased cartilage and bone, located at the head of the femur and acetabular cap, are replaced with artificial materials (a prosthesis).
More often than not, this is an elective procedure. Therefore, many older patients come to me for advice on whether or not to go for a THR. What I always tell them is that as with any surgical procedure there are potential risks, so it should not be entered into lightly and should be seen as a last resort. In my opinion, the biggest factor is how the operation will affect quality of life. If one’s current hip condition is impairing function to a significant extent – such that quality of life is severely diminished – then a THR would be of great benefit.
Who needs a THR?
- Patients with severe Osteoarthritis
- Patients who have tumours in the hip that have destroyed the hip joint rendering it dysfunctional
- In cases of avascular necrosis (hip joint is destroyed due to lack of blood supply) can develop due to fractures, drug and alcohol abuse and other diseases.
- Patients with intense chronic pain persists despite the use of anti-inflammatories for more than 6 months, adversely affecting sleep, ability to work and movement.
A THR is not recommended for patients with:
- A current hip infection
- Paralysis of quadriceps
- Severe blood disease
- Nerve disease affecting the hip
- Severe mental dysfunction
- Morbid obesity i.e. weighing more than 140kg
If possible, once one has decided to have the operation, it would be of great benefit to start pre-operative strengthening exercises to assist with rehabilitation post-surgery.
To prevent post operative risks, rehabilitation starts immediately after the operation. This includes circulatory and isometric exercises. On Day 1 post-surgery patients are usually sitting up, out of bed and working on strengthening the quadriceps. By Day 2 patients are walking with an assistive device (normally a walker). Physiotherapy is critical in the coming months to regain strength and functional activity.
For the first 3 months post-surgery it’s prohibited to lie on one’s side or cross one’s legs as the hip could dislocate in these positions. After 6 months normal daily activities should continue comfortably.
Always remember to inform your health care professionals that you have had a THR and avoid strenuous activities, running, contact sports etc as this will decrease the life span of your THR. Swimming is a very good way to strengthen and increase the mobility of your hip without causing too much strain on and friction at the joint.
Andrew Savvides
PhysioPRO
BY:
General Health/Fitness / Hip injuries / Lower Limb injuries

The trouble with being immobile
Our bodies were designed to move and participate in the different activities of daily living. So what happens when we, recovering from an injury or illness, find ourselves restricted to bed rest for a prolonged period of time? The way in which immobility affects our body and what we can do to prevent the associated complications, is worth exploring further.
Effect on the Cardiovascular system (heart and blood vessels)
Any activity of the muscles will push blood through your body. This blood flow through your veins and back to your heart will increase your circulation. So, when you are just lying in bed and not using those muscles, one risks peripheral oedema – swelling of your hands and feet.
Furthermore, being immobile for prolonged periods will see your resting heart rate increase as the heart needs to work harder to pump the blood through your body, without help from the body’s natural movement and muscle contractions. There will also be a decrease in the ability of the blood to take up oxygen, which can cause you to become dizzy or faint especially when u stand up after prolonged bed rest (postural hypotension).
Deep Vein Thrombosis is a serious complication associated with immobilisation. Which occurs due to an increase in the viscosity(thickening) and slowing down of the blood which basically forms a clot in the vessel. Dislodgement of a venous clot that lodges itself in the lung tissue is called a Pulmonary Embolism and may be fatal.
Effect on the Respiratory System
We all have fine little hairs in the airways that sweep secretions like mucous, phlegm etc upward and out of our respiratory systems. But immobilisation reduces the action of these cilia, or little hairs, and this inability to clear secretions may lead to infections such as pneumonia
Lung collapse (Atelectasis) – especially in the basal lobes of the lung – can also result as respiratory secretions accumulate in these lower lobes in the gravity dependent position and cause the small airways to close.
Effect on the Metabolic system
Prolonged bed rest causes the bones to lose calcium and potassium, as oesteoblastic activity(bone development) is reduced due to the lack of weight going throught the bones. This causes a decrease in the bone integrity or density of the bone matrix perhaps resulting in osteoporosis.
One may also develop kidney stones due to pooling of urine in the kidneys and bladder.
Effect on the Musculoskeletal system
It’s pretty obvious that if you not using your muscles that they will atrophy and weaken. Joint contractures – restrictions in the normal range of motion caused by peri-articular and intra-articular connective tissue – can occur. Basically your joints get stuck!
Another major complication of immobility is the possible development of pressure sores. These develop due to unrelieved pressure especially over areas where the skin lies close to bone. Pressure sores cause tissue death (necrosis). Once developed, these sores take a long time to heal and can be a source of secondary infection in the body.
Effect on the mind
To add to all these negative physical as well as physiological complications, being immobile affects one emotionally. People may have increased anxiety and depression and a decreased attention span.
What can you do?
Nearly all of these complications can be prevented with the right exercises and with help from your physiotherapist.
Undertake active circulatory exercises often, during the day, including foot pumping, static quadriceps and gluteal contractions, and active hip and knee exercises. These will all help to increase your circulation and benefit your cardiovascular system.
To deal with any respiratory problems work on increasing the efficiency of the lungs through deep breathing exercises and physiotherapy to the chest.
Weight bearing exercises are essential to prevent weakening of bones. Start getting out of bed and being mobile as soon as possible. While immobile, undertake exercise programmes that offer resistance training, either with your physiotherapist or using free weights.
As much active movement as possible should be facilitated, to make sure your muscles don’t weaken and shorten, always ensuring that the exercise is carried out to include its full range of motion to prevent contractures.
Ensure pressure relief, particularly on areas where the skin lies close to bone, by changing position every 2 hours, to prevent pressure sores and secondary infection.
It is also very important to try stay positive and motivated in this time of immobility. Speak to people, family, friends even your health care professionals. Set goals for yourself and your recovery and achieve them.
Until next time…Stay ACTIVE!
Andrew Savvides
PhysioPRO
BY:
General Health/Fitness
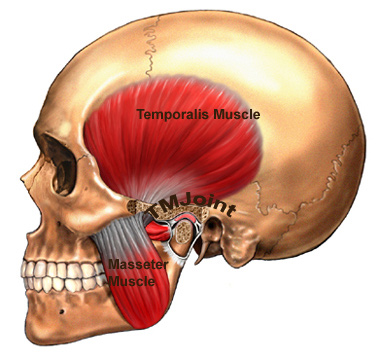
The TMJ- the little joint with a large role
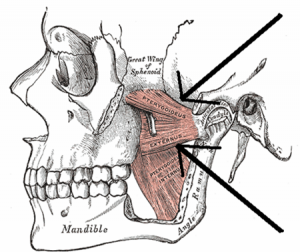
The Temporomandibular joint (TMJ) is a little joint with a big name and even larger role to play in day to day life. It’s found between the jaw bone and one of the bones in the skull – just below the temples.
When one considers how much we use this joint in daily activities it isn’t very surprising that this joint is subject to wear and tear. This, because it’s involved in chewing and talking (ceaseless activities for some). The TMJ can even be damaged while a person sleeps, as clenching or grinding one’s teeth will cause the joint’s cartilage lining to wear away.
Common causes of TMJ dysfunction are:
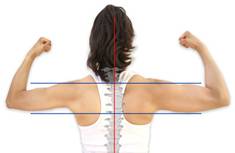
- Poor posture i.e. one that sees the chin poke out
- Habitual or excessive chewing of gum
- Previous trauma to the area
- Dental problems
- Stress and clenching of teeth
TMJ dysfunction could see people experience limited motion and a general dull ache over the side of the face as well as local muscle tenderness. A ‘click’ may also be present as patients open and close their mouth, as the joint dislocates and relocates back into place. Headaches, sinus and neck problems can all be associated with TMJ dysfunction. It’s clearly a very important joint to keep clear of damage.
A quick self test for TMJ health:
- Place 3 fingers vertically into your mouth. Inability to do this indicates TMJ hypomobility.
Using physiotherapy to treat damage to the TMJ involves:
- myofascial release
- massage
- gentle stretches
- accessory mobilizations
- electrotherapy
- postural correction
- re-education.
Most important is identifying and addressing the cause of the dysfunction.
So if you think you are having problems in this particular area, do not fear. Help is always at hand. Visit your PhysioPRO practice for an assessment.
Until next time…Keep Smiling 🙂 and chewing and talking.
Andrew Savvides
PhysioPRO
BY:
General Health/Fitness / Neck injuries

Effective ways to limit the risk of sports injuries
As all sports persons can attest, injury (or the risk thereof), and fear are the biggest concerns that may severely hinder performance and progression within sport. All sport carries an innate risk of injury, but it is very important for the sports enthusiast to bear the following in mind to limit the risk of injury moving into the new season…
It is essential to know where you are, to get where you want…
Do not overdo it from the get-go.
It is essential to know your current fitness level (which can be assessed by a physiotherapist), in order to plan and execute an appropriately graded training regimen moving into the season. The amount of training can play a key role in determining your injury risk. Fatigued muscles do a poor job of protecting their associated connective tissues, increasing the risk of damage to bone, cartilage, tendons and ligaments. In essence, when starting a new training programme, the loads of enthusiasm could lead to doing too much, too soon, increasing the risk of injury.
Warm Up Before Exercise
Many people are injured in the first few minutes in the gym, on the field or road etc, because they start too hard, without a proper warm-up. Always take 10-20 minutes to warm up gradually before going hard, especially before interval training or any high intensity form of training. A simple warm up can consist of brisk walking, jogging or simply doing your sport at a very slow pace to start.
Correct Diet for Exercise
Eating correctly is essential for energy to workout, a meal about 2 hours before exercise helps you get the most out of training sessions. Eating appropriately after exercise allows for tissue nutrition and optimal recovery for the next workout.
Drink enough water to stay well hydrated
Just a bit of dehydration will decrease your exercise performance which could then also lead to injury. Drink water according to the length and intensity of your exercise sessions. It’s recommended that you drink about 500-750ml water within two hours of exercise, and then drink a cup every fifteen minutes during exercise. If you exercise more than 90 minutes, you will need to add some simple carbohydrates (food or sports drinks) to replenish glycogen (stored glucose energy) stores.
Don’t Exercise with Pain
Exercise shouldn’t cause pain, stop exercising as soon as you experience acute or sharp pains. Pain is usually the body’s way of alerting us of some problem within the body. Pushing through this initial sharp pain may be a fast way to develop a severe or chronic injury. If you don’t feel well, it is a sign that you need some time off until your body heals.
With the repetitive pounding the body and its various systems take with training it is essential to allow time for rest. Rest is an essential component of the repair and regenerative process that leads to healing, growth and strengthening of new and previously damaged tissues.
Mix it up
Another way to prevent injuries is by cross training. Doing the same routine continuously lends the risk for overuse injuries, not to mention boredom and loss of focus. Training various muscle groupings also limits the risk of biomechanical injuries often caused by muscle imbalances. Cross train with other sports, yoga/stretching or resistance training as you can get a full body workout without over-stressing specific muscle groups.
Wear the Right Safety Gear for your Sport
It goes without saying that protective gear such as Helmets, protective pads, mouth guards, sun-glasses, and other specified gear designed to protect against common sports injuries are essential. Athletes should take advantage of this simple way to prevent the most common injuries. Never play without your recommended safety gear.
BY:
General Health/Fitness

Pedal Power
With summer on our doorstep and days getting longer and warmer many people are taking to the outdoors to find their fitness fix. And, what better way to enjoy this country’s spectacular natural areas and climate than through mountain biking or cycling. Many have set the annual 94.7 Cycle Challenge as their goal, and with the event around the corner beginners and experienced cyclists alike have been taking to streets and off-road trails in preparation.
Aside from knowing where the best spots are to enjoy a post-cycle breakfast, what else do cycling enthusiasts really need to know? Fitness and preparation for any sporting activity include understanding the associated risks – making this an opportune time to delve into common cycling injuries.
There will always be traumatic injuries that result from falls and other unplanned adverse events, the effect of which a physiotherapist will do their best to mitigate, to encourage healing. However what many physiotherapists deal with is the effect on the body of the repetitive motion and rhythm of cycling, which can cause what is called a repetitive strain injury due to incorrect biomechanics.
Common biomechanical faults:
- Forward head posture with craniovertebral extension (causing many cyclists to suffer neck pain)
- Thoracic kyphosis (the spinal curve being exaggerated due to the cycling position)
- Posterior pelvic tilt (the pelvis tilted backwards)
- Hip adduction and internal rotation (the hip turned inwards and across the body also due to the cycling position)
These postural problems can be minimized far in advance of commencing cycling by spending a little extra money on ensuring that a bicycle is set up correctly for an individual’s unique physiology – by a professional.
Something as simple as making sure your saddle is at the correct height and that your cleats are in the right position – and not rotated – can go a long way towards preventing much future discomfort and injury.
That said, the cycling position is not a natural one and following training in this position for extended periods of time many cyclists develop weakness of their hip extensors (which move hips backwards), their abductors (which move hips outward), lateral rotators (which turn the hips out to the side) and over activity of the hip flexors (which move hips forward), the adductors (which move hips inwards) and the medial rotators (which turn hips inward).
It is also very common for cyclists to have very tight calf muscles, which affects range of movement at the ankle making cyclists more prone to injury in that area. Remember to always stretch hip flexors, adductors, medial rotators as well as the calf muscles adequately before and after training.
It’s very important for cyclists to strengthen their hip extensors, abductors and lateral rotators. A very good way to do that is to start cross training i.e. exercising off the bike to target these muscle groups through other forms of exercise. It has also been shown that cyclists have a lower bone density -especially in the lumbar spine and hips – due to excessive calcium loss through sweating and all the hours spent on the bike. As cycling is a non-weight bearing activity it doesn’t promote an increase in bone density, but cross training – particularly doing weight-bearing exercises – will ensure bone density remains optimal.
Regards
Andrew Savvides
PhysioPRO
BY:
General Health/Fitness / Lower Limb injuries

Going bare…Part 2
One of the theories of man being adapted for barefoot running is that evolution once saw us as being persistence hunters. Man has a highly evolved thermoregulation and breathing system, whereas animals must pant to take in air to cool their organ systems. So, we were able to ‘run down’ our prey for several hours, resulting in the animal simply collapsing from sheer exhaustion and overheating (Persistence hunting)…Food for thought…
Although we appear adapted to running bare, there are definitely some Disadvantages of Barefoot (minimalistic) Running. Here we mention these cons…
If you have no problems and no pain, do you really need to change anything? … Why fix what isn’t broken?…
Glass, nails, rocks, thorns and other bits and pieces can injure our feet. Shoes save our feet and also offers protection from blistering (on hot surfaces) and frostbite (on cold surfaces).
Switching to a minimal shoe or starting to go shoeless will usually result in blisters for the first few weeks until calluses are formed.
For most of us modern athletes, going minimalist will be a shock to our feet and our running system of muscles and joints will be overwhelmed. This could lead to injuries such as Achilles tendinitis, calf strain or medial knee pain when the typical heel lift is removed from the shoes.
The sole of the foot (plantar surface) is usually soft and tender. Going without a generously soled shoe may initially cause plantar pain, and raise the risk of plantar fasciitis (inflammation within the sole of the foot).
And…let’s face it: It looks a little strange, so people will notice, and they may stare 🙂
BY:
Foot injuries / General Health/Fitness / Lower Limb injuries

OUCH
The most annoying of all injuries is probably knocking your little toe into a piece of furniture or door frame… However the most common everyday injury is the Ankle sprain…
The ankle joint, which connects the foot with the lower leg, is often injured in an unnatural twisting motion that occurs when the foot is planted awkwardly, when the ground is uneven, or when an unusual amount of force is applied to the joint. Ankle sprains are common sports injuries but can also happen during everyday activities such as walking or even getting out of bed.
The ankle joint is complex and comprises of several bones, many ligaments and tendons.

Ligaments are injured when a greater than normal stretching force is applied to them. This happens most commonly when the foot is turned inward or “inverted”. Outward or “eversion” sprains are less common, but usually more severe. Both results in tissue injury and inflammation. Blood vessels become “leaky” and allow fluid to ooze into the soft tissue surrounding the joint. White blood cells responsible for inflammation migrate to the area, and blood flow increases, all causing signs of inflammation: swelling, pain, tenderness, redness and warmth…
Urgent medical attention should be sought if signs appear more serious than this, for e.g., pain is excessive, despite the use of medications, elevation, and ice; the person cannot walk at all or cannot walk more than a few steps without severe pain, and/or the foot or ankle is excessively swollen. Fractures can also occur during severe sprains, and your physiotherapist can advise you when an x-ray is necessary.
Less severe sprains can be handled by self care at home by aiming to reduce and prevent inflammation…Remember PRICE: protect, rest, ice, compression and elevation (see Acute Injury Management blog).
Simple ankle sprains usually resolve between 6-8 weeks, however people often experience residual pain and stiffness in the ankle without proper rehabilitation. The chance of re-spraining the same ankle is said to be close to 80% due to a lack of, or improper rehabilitation. To avoid this and gain complete recovery, seek expert care and rehabilitation of the ankle from a physiotherapist.
Physiotherapy treatment options for ankle sprains
Depending on the results of your ankle evaluation and examination and your specific needs and goals, your physiotherapist will create a comprehensive treatment plan specifically made for you. Physiotherapy treatments may include a combination of the following
- Patient education
- About the condition
- Precautions and injury prevention
- Work or activity modification
- Home treatments for symptoms
- Home exercise program
- Recommend bracing or immobilization
- Recommend walking device (e.g. cane, crutches)
- Kinesiology Taping, Sports taping/Bandaging
- Ice / Heat application
- Electrotherapy & Ultrasound (US)
- Joint mobilization
- Graded Physiotherapy exercises including Balance, Proprioception and Gait re-education
- Formulate a work or sport-specific ankle rehabilitation program
The physiotherapy treatments for ankle sprain listed above will not be provided to you in one visit. Your physiotherapist is your best source for which interventions are best for you, based on your specific problems, overall level of fitness and your goals.
So if you have sprained your ankle already, or would just like to prevent this injury from occurring, pop in to your nearest PhysioPRO today.
Mitesh@PhysioPRO
BY:
Ankle injuries / Lower Limb injuries

The CORE of the matter
Many patients come to my practice having heard something about inner core stability, but the majority have a very skewed perception of the core muscles and how to exercise these.
As an example, I asked a patient of mine (a provincial rugby player) if he does core exercises. “Yes”, he replied, “I do 100 crunches every day!”
You may think that this is the ideal response, but in fact he had very poor core stability when tested, and by the end of this article you should realise that he was in fact not training his core muscles.
To understand the concept of the “core”, one first needs a basic understanding of the muscles that make it up. The core can be related to a cylindrical can.
- The lid of the can is the diaphragm
- The bottom is the pelvic floor
- The front and sides are made up of a deep stomach muscle (you’ve probably never heard of it) called Transversus abdominis
- Lastly the back is a muscle called Multifidus
These muscles all act together to increase the pressure inside the stomach cavity, and in so doing increase stability around the mid-section. A good way of visualising this is to try imagine squeezing a new tube of toothpaste with the cap on. The tube keeps its basic shape and is quite difficult to compress. Now remove the cap or make a hole in the side of the tube and suddenly the tube collapses.
The deep stomach muscle and Multifidus also have connections to the spine itself and when contracting, prevent excessive movement at the spine during activity.
So why was the rugby player not training his core you ask?
Well, most people only train the top three layers of stomach muscles during regular stomach exercises. Crunches, sit-ups and similar exercises all involve movement of the torso and so you tend to only train the “mobilising” muscles. These may look good when your shirt is off, but do very little for your back. The deep stomach muscle is a “stabilising” muscle, so in order to train it, you need to challenge your bodies’ stability.
This is where Physio-balls, Bozu-balls (half a physio-ball) and Pilates come in. Using this equipment under the supervision of a trained Physio or other health professional will help you train your core correctly by challenging your balance and stability. Most of the exercises that use this equipment will be static exercises (i.e. holding a certain position with as little movement as possible) and then at a more advanced stage, movement can be added. Ever seen a person doing a full squat whilst standing on a Physio-ball? These people have phenomenal core stability and its quite amazing to watch.
One last thing worth mentioning is that if you do go to Pilates, PLEASE make sure your instructor shows you how to isolate Transversus Abdominis before you commence any exercises. If you have not been shown how to do this, you could do more harm than good. For this reason, Pilates classes at the gym down the road is probably not the best place to start this form of exercise unless you can get individual attention.
There is so much more to be said about core stability and its importance, but I hope this short explanation will help you to better understand your body.
If you need more info or would like to check and train your core, give us a call and let us bulletproof your back.
Ric@PhysioPRO
BY: Riccardo Vaccaro
General Health/Fitness / Lower Limb injuries / Upper Limb injuries