Acute injuries- RICE or MEAT?
Things are constantly evolving in the world of sports medicine. With a better understanding of how the human body works, comes an ever changing understanding of how best to treat it. One such notion which needs to be challenged is the age old acronym of R.I.C.E (Rest, Ice, Compress, Elevate) used for the management of acute injuries.
The “Rest” part of this strategy may in fact cause delayed healing and muscle atrophy. Several studies that have compared early PAIN-FREE movement to complete rest have shown decreased healing times and improved pain.
As I stated above, what is quite important is to start moving early on, but specifically without pain. Even some serious injuries/operations should allow for a degree of movement that is pain free.
Another area of uncertainty is the application of “ICE”. Whilst there is evidence that ice causes a numbing effect on tissue (by decreasing the speed and transmission of nerves), thereby reducing pain, the notion that icing decreases the inflammatory response and speeds up healing is being challenged.
Some studies are showing that the application of early ice (for 20 minutes in the acute stage of an injury) may in fact reduce the healing potential of tissue, and cause longer term negative effects on the healing collagen. So if your intention is to reduce pain, then ice may be appropriate, but if you think you are assisting the body healing process, think again…

What is now being suggested is a new acronym – M.E.A.T
MOVEMENT – as discussed earlier, must be pain-free
EXERCISE – the correct exercises done early on have been shown to reduce muscle wasting and improve outcomes
ANALGESICS – used to control acute pain, but be careful not to “mask” the pain so you can go back to activity too quickly. Again, avoid anti-inflammatories at first.
TREATMENT – from a Physiotherapist or other sports medicine practitioner. We can use other modalities to improve circulation and assist healing.
The Editor in Chief of The Physician and Sports Medicine Journal was quoted as saying,”Do you honestly believe that your body’s natural inflammatory response is a mistake?” I’ve said it in my article on anti-inflammatories, the first stage of healing is INFLAMMATION, but it seems we have all been hell-bent on trying to stop this.
It would appear that the more we learn about how to heal the human body, the more we realise it does a pretty good job, all on its own!
Ric@PhysioPRO
BY: Riccardo Vaccaro
Ankle injuries / General Health/Fitness / Knee injuries

We will, we will SHOCK you!!
Shock wave therapy (also known as extracorporeal shock wave) is a cutting edge form of treatment in the world of sports medicine. Its a very similar technology to that used to “blast” kidney and gallstones, and does not involve electrical shocks (don’t panic, this isn’t the dark ages) but rather mechanical pulses, similar to sound waves.
Although the physiological mechanism of how exactly this mechanical pulse works is still not fully understood, the research shows us that the “waves” cause microtrauma and inflammation, stimulating the formation of new blood vessels and nerve cells, and speeding up healing of tissue. There is also a positive effect on reducing pain through a pain gate mechanism.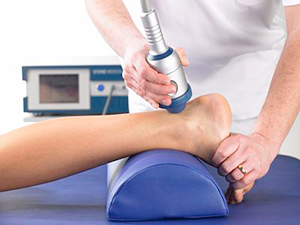
In other words, it improves blood supply and speeds up tissue regeneration!
So why is this so amazing you ask?
Well basically its taking something the body would normally do on its own, and speeds it up significantly, without the need for injections or surgery. Numerous medical research reports have shown that shockwave therapy can be 80-90% effective at completely and rapidly resolving injuries within 3-6 applications.
The most significant application in sports medicine is in the treatment of chronic tendon, muscle and joint conditions. So things like:
- Tennis elbow/ Golfers elbow
- Rotator cuff tendinopathy
- Frozen Shoulder
- Trochanteric Bursitis
- Hamstring tendinopathy
- Achilles tendinpathy
- Patella tendinopathy
- Plantar fasciitis
- Muscle knots and trigger points
- ITB friction syndrome
- Chronic ligament pain
- And even more conditions are healing in weeks instead of months…
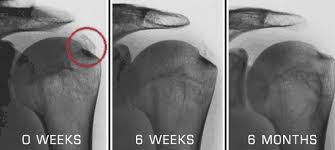
It is particularly effective in breaking down the calcification of tendons, commonly seen in the shoulders, as can be seen in the x-rays below…
As technology and techniques improve, so will we find new uses for shock wave therapy. In fact, I chatted to a Doctor at one of the top SA rugby teams, who said they use shock wave to treat nearly all injuries on their players and are getting fantastic results.
Already studies show that in bone fractures that either wont heal quickly, or at all, the application of a single shock wave treatment was effective in causing fracture healing in 87% of patients.
It also has applications in the healing of diabetic foot ulcers, treating cardiac chest pain and erectile dysfunction…but don’t come to me for that!
So if you, or anyone you know has one of the above conditions, give us a call to see if Shock Wave Therapy might be the treatment for you…
Ric@PhysioPRO
BY: Riccardo Vaccaro
Ankle injuries / Elbow injuries / General Health/Fitness / Knee injuries / Shoulder injuries

Increase your running distance safely
How to safely increase your running distance
With summer just around the corner, most people have started getting ready for their beach body. You may have taken up any number of sports to achieve this, but certainly, the most common “seasonal sport” is running. Running is a relatively cheap, easily accessible sport, but if you are not careful with how you increase your distance it could turn into a costly exercise…
Most runners have heard of the 10% rule. This states that you should never increase your distance by more than 10% from the previous week. This “rule” has not been validated by science and a recent article published in the Journal of Sports and Orthopaedic Physical Therapy, revealed some interesting findings.
The study followed 874 novice runners for 1 year and gave each runner a GPS watch to track their distance. Based on their weekly running increase, they were placed into one of three groups: less than 10%, 10%-30% and more than 30%. In total 202 participants sustained an injury over the course of 1 year and what will surprise most is that the total number of injuries per group were not much different.
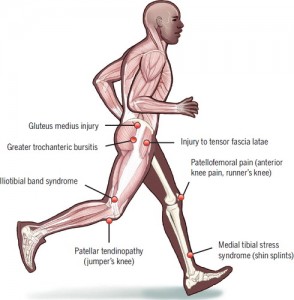
Yes, there was an increase in the number of distance related injuries in the group that increased by more than 30% compared to the group that increased by less than 10%. So injuries like patellofemoral pain (runners knee), iliotibial band syndrome, medial tibial stress syndrome (shin splints), gluteus medius injury, greater trochanteric bursitis, injury to the tensor fascia latae, and patellar tendinopathy (jumpers knee) were more common in the group that increased training distance by more than 30%.
A possible explanation for this is that when you increase your distance, your running speed decreases (especially if you get fatigued). If your speed decreases, you have to take more steps to complete a given distance and the increased number of steps equates to increased “wear and tear”.
However, this was not true for all injuries. Injuries like plantar fasciitis, Achilles tendinopathy, calf injuries, hamstring injuries, tibial stress fractures, and hip flexor strains were just as common in all 3 groups. These injuries may be linked to running pace rather than distance, and its only through more research that these answers will be revealed.
So, all that science can presently advise is that you progress your weekly distances by less than 30% per week over a 2-week period.
Train smartly!
Ric@PhysioPRO
Article by Rasmus et al, titled “Excessive Progression in Weekly Running Distance and Risk of Running-Related Injuries: An Association Which Varies According to Type of Injury” J Orthop Sports Phys Ther 2014;44(10):739-747. Epub 25 August 2014. doi:10.2519/jospt.2014.5164
BY: Riccardo Vaccaro
Ankle injuries / Foot injuries / Hip injuries / Knee injuries / Lower Limb injuries
Lower Back Pain
Lower Back Pain…Where is it coming from?
Lower back pain is a common injury seen at my practice, both in the sporting and non-sporting population. There are multiple pain producing tissues of lower back pain (muscles, facet joints, ligaments, fascia etc) however, two of the most commonly affected tissues are the disc and nerve. This short article should give you an idea of the difference in symptoms between the two structures.
What is the disc?
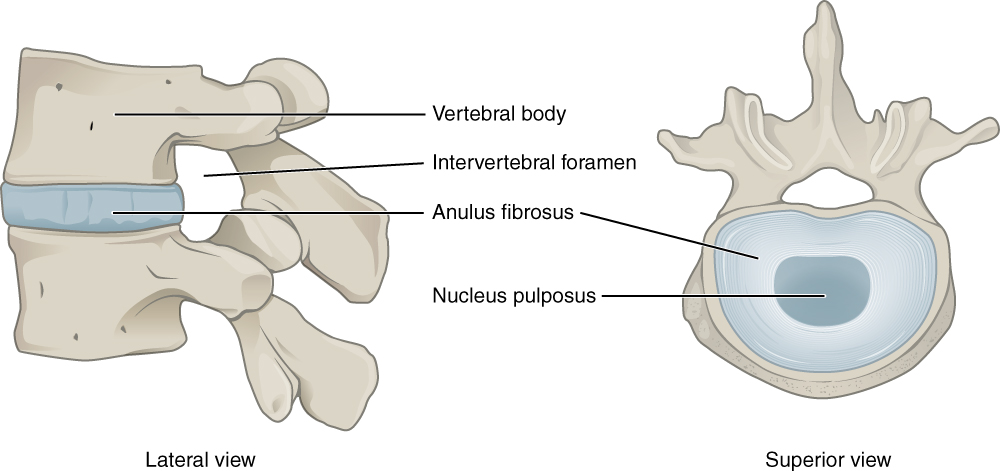
The Intervertebral Disc, is made up of two different tissues…On the outside, we have a thick, tough ring called the Anulous Fibrosus, and on the inside, we have a “jelly-like” material called the Nucleus Pulposus. The disc sits between two vertebral bodies and is not a true “joint”, but acts as more of a shock absorber and allows for one vertebra to move on another. I often tell my patients to imagine a thick layer of jam between two pieces of hard toast. If you squash the toast on one side, the jam gets pushed out the opposite side. For example, when you bend forwards, the jelly inside gets squashed and moves backwards, allowing the two vertebra to move, but not “collapse”.
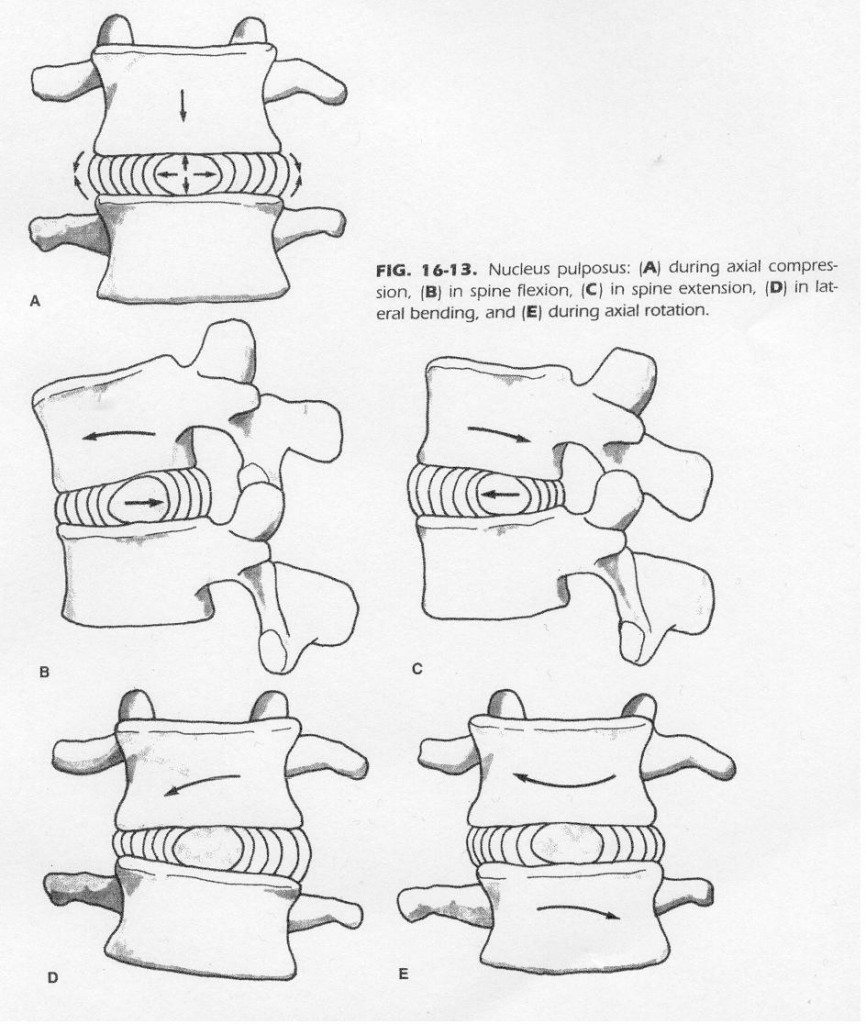
The problem occurs when we put too much loading through the disc, and then force the jelly in a certain direction. A typical example of this is when you bend over to move a heavy box and then you are unable to stand up straight due to the pain in your lower back. The position of the jelly combined with the added weight of the box causes the jelly to be forced backwards and it pushes into the outer ring (see images 1 and 2 below).
This is referred to as a DISC BULGE and can be compounded by a small amount of wear-and-tear of the outer ring (small tears and cracks with ageing). Symptoms of a disc bulge include a broad “band” of pain across the lower back (and sometimes into the buttock) as well as sharp pain with changing positions (sit to stand). Coughing and sneezing are often painful (due to the increase in abdominal pressure, pushing the disc material out further). Usually these disc bulges heal well with physiotherapy techniques (we try to gently squeeze the damaged tissue back in) and anti-inflammatories, and depending on the extent of the damage, can take anywhere from a few days to a few weeks to heal…
If the injury is more severe, we speak of a DISC HERNIATION (Image 3- it has now broken through the outer ring) OR DISC SEQUESTRATION (image 4- part of the jelly has “broken away”). At this point, the inflamed disc and its material often starts to push on the nerve exiting the spine, and now we also have NERVE ROOT IMPINGEMENT.
This is usually accompanied by pain, numbness, weakness and pins/needles of the affected nerve root (pain usually radiates down a part of/or the whole leg), and the pain in the leg usually outweighs the pain in the lower back. These injuries take longer to heal and conservative therapy does have a high rate of recovery, however surgery is sometimes needed.
A nerve can also get trapped where it exits the spine through a little opening called the foramen. Generally this happens in older patients with arthritic degeneration, where the opening becomes narrower due to extra bone formation, enlarged joints and narrowed discs. This produces similar symptoms of pain, numbness and pins/needles but generally, the symptoms gradually appear and get worse with time.
Hopefully this helps you have a better understanding of whats going on in your back.
Ric@Physiopro
BY: Riccardo Vaccaro
Back injuries

Take this pill-tear that muscle!
So you go to see your doctor because you have the flu. The doctor books you off and prescribes antibiotics. One or two weeks later you start to feel better so you decide to go for a jog, and thats when it happens! Suddenly you hear a loud “crack” and start limping. You’ve TORN your achilles tendon and you weren’t even straining yourself?
This same scenario has happened to many people and its not because they were sick or unfit, its because of the ANTIBIOTIC that was prescribed!!!
A group of Antibiotics called Flouroquinolones are associated with a wide variety of musculoskeletal problems that affect muscle, tendon, bone and cartilage. They are commonly used to treat a variety of urinary tract, digestive, respiratory and skin infections amongst others. In the USA, this class of antibiotic is THE most prescribed type to adults, even though since as early as 1983 it was known that this drug was toxic to musculoskeletal tissue. Symptoms have been known to occur as early as 2 hours after the initial dosage and as late as 6 months after!!
In one study of 42 patients who developed Tendon related problems, 76% experienced tendinopathy (sick tendons) and the other 24% had complete ruptures of the tendon. Muscle symptoms range from mild muscular pain to a very serious and life threatening condition known as Rhabdomyolysis. Bone problems are less conclusive in humans, but in animal studies, it has been shown to slow down or even stop a bone from repairing itself.
What they have discover in more recent times is that there are factors which make you more at risk of developing these symptoms. These include: increasing age, use of cortisone, playing sport, a previous history of tendon or joint problems, magnesium deficiency and diabetes to name but a few.
So what should you do or how can this be avoided?
Not to discredit any Doctor or other health professional, but if you are being prescribed an anti-biotic, check with them that this will be safe to use, especially if you are a physically active person. I had a patient recently that developed general muscle ache, along with severe elbow pain for no apparent reason. She had all the symptoms of someone that had trained heavily the past few days, which she hadn’t. She also had Tennis elbow symptoms and it turned out she was prescribed a Flouroquinolone by her dentist for a tooth infection the week before…
So your doctor should get a thorough history of your previous musculoskeletal problems, find out about your activity levels, ask about associated risk factors and advise you to stop the drug immediately if it is causing any symptoms.
If you are an Athlete, you should definitely not be using this class of antibiotic unless there is no available alternative drug. If you are presently taking this drug, or have used it in the past 6 months, reduce your training intensity, avoid ballistic movements and be aware of any development of symptoms.
Ric@PhysioPRO
Full article by Hall et al. Published in the American Academy of Physical Medicine and Rehabilitation, Vol 3. 132-142, Feb 2011.
BY: Riccardo Vaccaro
General Health/Fitness

Modified Shoulder Stretches
Sometimes just by modifying the position or way you perform a stretch slightly, you can have much better results and outcomes. So when I came across an article about two modified shoulder stretches, I just had to share it with all of you.
Two of the most commonly used shoulder stretches to increase the flexibility of the posterior soft tissues are the cross-body and sleeper stretch exercises. But, based on the inability to stabilize the shoulder blade and control glenohumeral joint rotation with the cross-body stretch and the potential for subacromial impingement with the sleeper stretch, it has been recommend that modifications to both of these commonly performed stretches be made.
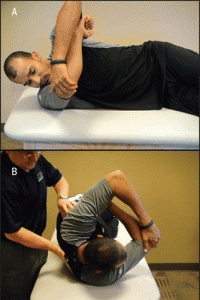
The modified sleeper stretch is performed with the athlete in a sidelying position, trunk rolled posteriorly 20° to 30°, and shoulder elevated to 90°. In this position, the athlete passively pushes his forearm down towards the bed using the opposite arm, a towel may also be placed under the arm of the stretched limb. This modified sleeper stretch position puts the posterior structures of the shoulder under more tension thus making it more effective.
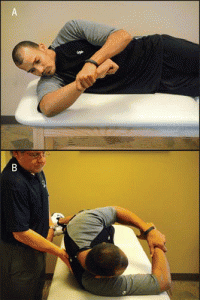 The cross-body stretch is often performed with the athlete in an upright standing position, using the opposite hand to horizontally adduct the targeted shoulder (pull your arm across your body).
The cross-body stretch is often performed with the athlete in an upright standing position, using the opposite hand to horizontally adduct the targeted shoulder (pull your arm across your body).
This method has the disadvantage of not providing stability to your shoulder blade and allows excessive external rotation of your shoulder. Due to this optimal stretch of the posterior shoulder is not achieved. Therefore, to better stabilize the shoulder blade, it has been suggested that the athlete be in a sidelying position, and, to restrict external rotation of the shoulder,the athlete should align the forearms together with the opposite forearm on top.
Well I hope these little adjustments to your stretching techniques yield large results.
Andrew@PhysioPRO
Reference: Journal of Orthopaedic & Sports Physical Therapy, 2013, Volume: 43 Issue: 12 Pages: 891-894
BY:
Shoulder injuries / Upper Limb injuries

Glorious Gluteus Muscles!
Back in 2011 I wrote an article called “How your BUM controls your BODY”. In the article I explained why the gluteus muscles are such an important muscle to train because it directly affected your ankles, knees and hips. If you haven’t already read it, then I suggest you go read it by clicking here.
In about 90% of lower leg injuries, I find that these gluteus muscle needs strengthening, so its crucial if you have any of those conditions mentioned in the previous article. In the article I only showed one exercise to do that targeted that gluteus muscle. Today I want to give you some more so you can really work it.
Advanced Clam
The starting position for this exercise is much the same as for the original Clam shell exercise (lying on your side,knees bent and heels touching). Place your forearm on the floor and then “push” your bottom knee into the floor, forcing your body to lift up off the floor-similar to a side plank. Now move the top knee up and down, but keep the heels touching.
The difference here is that you are training BOTH bum muscles at the same time. The bottom leg’s bum muscle is having to hold you up whilst keeping static (isometric) whilst the top leg’s bum muscle is moving the top leg (concentric). Trust me, it’s a real killer and you should feel the burn in your bum, right behind your hip. Once you can do 3 sets of 15 reps, then try adding an elastic band around your knees. An added advantage of this exercise is that is also trains your core at the same time!
This one looks easy but don’t be fooled… Stand with one leg over the edge of a step. Now keeping both knees LOCKED OUT STRAIGHT, lower your one leg by dropping your pelvis down on that side (keep those knees straight!). Now lift that leg as high up as you can and repeat. You want to concentrate on slowly lowering the leg (eccentric movement), and you should feel a burn in the gluteus muscle of the leg that you are standing on. Again, do 3sets of 10-15, but the slower you go the better.
So there you have it, two more exercises to add to your prevention program! And to all my CrossFit Athletes, this WILL help with your squat form! Tight buns
Ric@PhysioPRO
BY: Riccardo Vaccaro
Foot injuries / Hip injuries / Knee injuries / Lower Limb injuries

Osgood-Schlatter lesion
Anterior knee pain is a common complaint among sportsmen. One of the main causes of anterior knee pain in younger athletes is a condition known as Osgood-Schlatter lesion.
This condition is extremely common in teenage boys with a high level of physical activity, generally occurring at the time of a growth spurt. Mainly associated with sports involving a lot of running and jumping e.g. basketball, soccer, gymnastics etc.
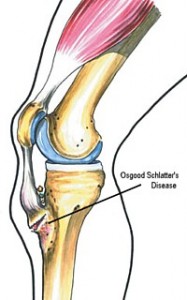 Examination reveals tenderness and pain over the tibial tuberosity (a small outgrowth on the shin bone where the patellar tendon attaches), with associated tightness of the quadriceps muscle. Excessive subtalar pronation (flat feet) may predispose the adolescent to the development of this condition.
Examination reveals tenderness and pain over the tibial tuberosity (a small outgrowth on the shin bone where the patellar tendon attaches), with associated tightness of the quadriceps muscle. Excessive subtalar pronation (flat feet) may predispose the adolescent to the development of this condition.
The pain is mostly aggravated by exercise and thus the management of the condition requires the athlete to modify their activity levels i.e. the less activity they do, the less pain they will have. Osgood-Schlatter lesion is a self-limiting condition, which means with time it will resolve by itself but may take up to 2 years. This can be very frustrating for the athlete and parents especially if they do not understand the nature of the condition. In the long term the athlete may develop a thickening and prominence of the tibial tubercle which will present as a bump on their shin bone just below the knee.
When the athlete is suffering from pain the symptomatic management includes icing the region, electrotherapy, massaging and releasing the quadriceps muscle, stretching as well as correcting any subtalar pronation if present.
So if you are suffering from this condition head to your local physiotherapist for advise and treatment.
Andrew@PhysioPRO
BY:
Knee injuries / Lower Limb injuries

Putting your Back Pain to Bed
Im often faced with patients that are suffering from lower back pain for one or other reason. Part of my usual advice is on how to find a comfortable position so that you can get a decent nights rest…
Sleep is an integral part of the bodies ability to heal, so when you are being kept awake due to pain, you often feel worse, your nervous system is more “on edge” and you are generally more miserable from this. As a result, you feel more pain and then cant get the sleep you need. Its quite a vicious cycle…
So to start with, the basic principles of getting some decent shut-eye is to place the least amount of strain on the lower back. By that i mean having the back in a “neutral” position where it is neither rotated nor over extended/flexed.
So here they are:
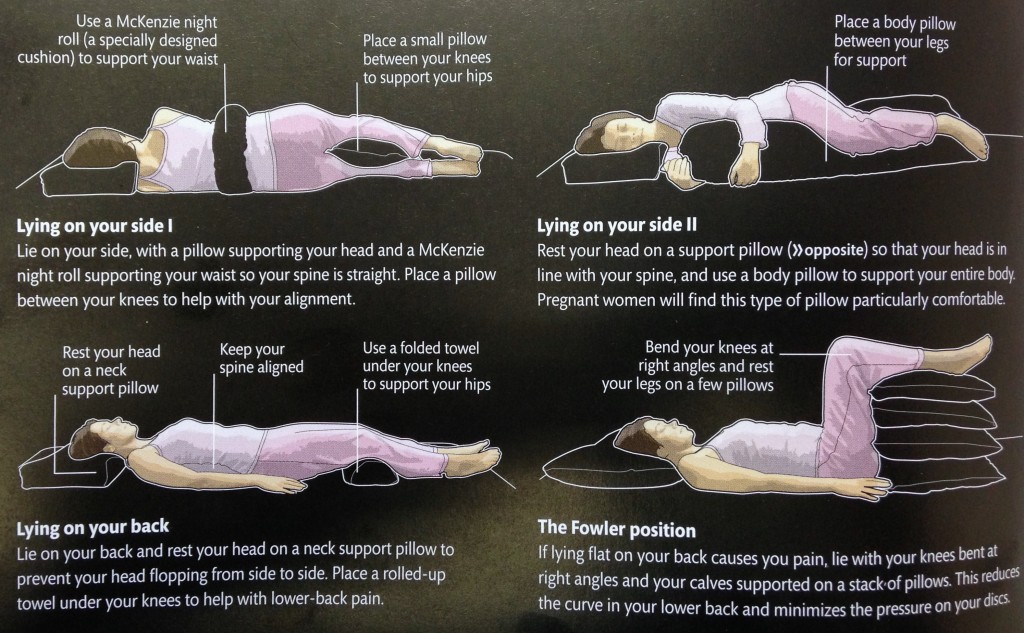
TOP LEFT- Lying on your side with a pillow between the knees. The height of the pillow does matter here. If you lay with both knees bent, then a small pillow should fill the “gap” between your knees, however if one knee is bent and the other is straight (TOP RIGHT), a bigger pillow is required. You could also place a soft pillow or rolled up towel under your side to fill the gap between hip and ribs.
Or try lying on your back with 1-2 pillows under the knees (BOTTOM LEFT). If this doesnt help alleviate your pain, then up to 4 pillows (BOTTOM RIGHT) can be used to get comfortable. This helps flatten the lower back and also reduces the stretch normally placed on a muscle connected to your spine (iliopsoas).
So there you have it, and I hope it helps you get a good nights rest!
Ric@PhysioPRO
BY: Riccardo Vaccaro
Back injuries